| Heart failure is a serious medical condition where the heart does not pump blood around the body as well as it should, which causes a fluid to accumulate in lungs and other parts of the body. However, if recognized on time, and adequately treated, patients can have a long and a good quality life. Heart failure often develops because you have (or had) a medical condition, such as coronary artery disease, a heart attack, high blood pressure, heart valve disease, heart muscle disease, inflammation of the heart or congenital heart defects which has damaged or put extra workload on your heart. It is essential for patient to keep a good track of symptoms notify a physician as soon as any change develops.
 SHORTNESS OF BREATH is caused by fluid accumulation and congestion in the lungs. In the early stages of heart failure you will probably only experience breathlessness after exercise, but later when resting as well. If you do feel breathless at night or when lying down, try supporting yourself with pillows so you are lying in a more upnght position. If symptoms persist, the correction of therapy is necessary. COUGH OR WHEEZING usually develops due to fluid accumulation in the lungs, but can also be caused by lung conditions (such as chronic obstructive pulmonary disease (COPD) and asthma). SHORTNESS OF BREATH is caused by fluid accumulation and congestion in the lungs. In the early stages of heart failure you will probably only experience breathlessness after exercise, but later when resting as well. If you do feel breathless at night or when lying down, try supporting yourself with pillows so you are lying in a more upnght position. If symptoms persist, the correction of therapy is necessary. COUGH OR WHEEZING usually develops due to fluid accumulation in the lungs, but can also be caused by lung conditions (such as chronic obstructive pulmonary disease (COPD) and asthma).
It is very common for people with heart failure to experience rapid CHANGES IN THEIR WEIGHT is caused by fluid accumulation or fluid loss after appropriate treatment. It is important to weigh yourself and tell your doctor if you notice your weight increase by more than 2 kg in 3 days.
 SWELLING ANKLES. Fluid accumulation can cause swelling (edema), particularly in the ankles. Sometimes the swelling can extend into your legs, thighs and abdomen. Your doctor or nurse may recommend limiting how much you drtnk every day, in order to limit the amount of fluid that can build up in your body. He/she may also recommend that you take an extra diuretic when required. LOSS OF APPETITE. Fluid accumulation in liver and digestive system can make you feel full and/or bloated. Therefore, you may feel less hungry. You can try eating smaller meals more frequently. SWELLING ANKLES. Fluid accumulation can cause swelling (edema), particularly in the ankles. Sometimes the swelling can extend into your legs, thighs and abdomen. Your doctor or nurse may recommend limiting how much you drtnk every day, in order to limit the amount of fluid that can build up in your body. He/she may also recommend that you take an extra diuretic when required. LOSS OF APPETITE. Fluid accumulation in liver and digestive system can make you feel full and/or bloated. Therefore, you may feel less hungry. You can try eating smaller meals more frequently.
NEED TO URINATE AT NIGHT. When you lie down in bed at night, the fluid that has built up in your legs dunng the day can move back into your bloodstream and is taken to your kidneys to be eliminated as waste unne. Going to the toilet before going to bed and limiting the amount you drink in the evening may help reduce the number of times you have to get up at night to urinate. Taking your diuretic in the morning may also help.
|
DEPRESSION AND ANXIETY. It is very common for people with heart failure to feel depressed, uneasy or anxious. Heart failure symptoms can leave you worn out and exasperated and may prevent you from participating in normal social activities
 TIREDNESS I FATIGUE. The lack Of oxygen and nourishment cause your muscles to get tired much more quickly. Moderate exercise and exercise training may help improve your symptoms. TIREDNESS I FATIGUE. The lack Of oxygen and nourishment cause your muscles to get tired much more quickly. Moderate exercise and exercise training may help improve your symptoms.
DIZZINESS. Dizziness in people with heart failure is often caused by their medicines. However, irregular heartbeats, which often happen with heart failure, or a temporary drop in blood pressure caused by nsing from a sitting or lying position can also cause dizziness.
RAPID HEART RATE. When you have heart failure, your heart tries to compensate for its lack of pumping power by beating faster (tachycardia) in order to keep up the same flow of blood around your body.
WHAT CAUSES HEART FAILURE?
Heart failure can be caused by current or past medical conditions, which damage or add extra workload to the heart:
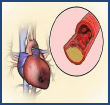 HEART ATTACKS are the fnost common cause of heart failure. During heart attack one of the arteries supplying heart muscle becomes completely blocked, cutting off the blood supply, oxygen and nourishment to heart muscle, causing it to die. Your remaining healthy heart muscle then has to pump harder to compensate, putting more workload onto your heart than it can handle. HEART ATTACKS are the fnost common cause of heart failure. During heart attack one of the arteries supplying heart muscle becomes completely blocked, cutting off the blood supply, oxygen and nourishment to heart muscle, causing it to die. Your remaining healthy heart muscle then has to pump harder to compensate, putting more workload onto your heart than it can handle.
CORONARY ARTERY DISEASE. In coronary heart disease, one or  more of your coronary arteries has become narrow due to the buildup of a cholesterol containing mass (plaque) inside the artery wall. This narrowing of your artery reduces the amount of oxygen and nourishment that are able to reach your heart muscle, causing angina (chest pain). This can be delayed or even prevented by lifestyle and medical approaches. more of your coronary arteries has become narrow due to the buildup of a cholesterol containing mass (plaque) inside the artery wall. This narrowing of your artery reduces the amount of oxygen and nourishment that are able to reach your heart muscle, causing angina (chest pain). This can be delayed or even prevented by lifestyle and medical approaches.
HIGH BLOOD PRESSURE causes your heart to pump harder than normal to keep the blood circulating. Hypertension that is not controlled increases your risk of heart failure. Hypertension can be easily treated.
HEART VALVE DISEASE, HEART MUSCLE DISEASE OR INFLAMMATION OF THE HEART AND CONGENITAL HEART DEFECTS. If your valves don't work properly, they don't close and/or open completely during each heartbeat. Your heart has to work harder to keep enough blood moving in the correct direction and heart failure may develop. Cardiomyopathy changes the structure of your heart. The muscle may thicken and become stiffer, or the heart may dilate. Myocarditis is an acute inflammation of your heart
|
muscle, usually caused by a viral infection that may result in a dilated cardiomyopathy. If your heart and its chambers weren't formed correctly before you were born, the blood flow in your heart or vessels near it may be blocked or have abnormal pathways or connections. This makes it harder for your heart to pump blood around your body and the extra workload can cause heart failure.
LUNG, KIDNEY AND OTHER CONDITIONS. If you have lung disease, there is less oxygen in your blood and your heart will have to work harder to deliver the available oxygen around your body, which can cause heart failure. Heart failure caused by lung disease usually affects the right side of the heart and it usually causes fluid accumulation in your legs and abdomen. When kidneys are diseased or not functioning properly, they produce hormones that retain salt and water even when blood volume has increased, causing further fluid accumulation and congestion. Other conditions, such as, infection , anemia, abnormal heart rhythm, diabetes and overactive thyroid gland may aggravate heart failure
COMMON TESTS FOR HEART FAILURE include: Medical history, Physical examination. Electrocardiogram (ECG), Blood tests. Chest x-ray, and Echocardiogram. Additional tests may be able to find out more about your heart failure or identify the cause that include: lung function tests, exercise testing, cardiac Magnetic Resonance Imaging (MRI), cardiac catheterization and angiography, nuclear medicines techniques and Multi-slice Computer Tomography (MSCT).
HOW CAN HEART FAILURE CHANGE OVER TIME? Heart failure is a serious, chronic condition that tends to gradually get worse over time. Eventually it can shorten your life. The careful management of your condition can not only ease symptoms but can also improve prognosis and prolong life.
HEART FAILURE MEDICINES Depending on your symptoms, general health and lifestyle the available groups of heart failure medicines are: Diuretics, ACE (Angiotensin converting enzyme) inhibitors, ARBs (Angiotensin II receptor blockers). Beta blockers. Aldosterone receptor antagonists. Vasodilators, Digitalis preparations. Antiarrhythmics, Anticoagulants, Antiplatelets and Statins.
DEVICES AND SURGERY. If you have an abnormal heart rhythm or if the electrical impulses do not travel through your heart properly, the implantation of special devices called pacemakers is necessary that improve symptoms and long- term survival. Sometimes, it may be necessary for you to have stent implantation or heart surgery such as coronary artery bypass, valve replacement surgery and heart transplantation.
HELPING YOURSELF
ADAPTING YOUR LIFESTYLE. Heart failure is a chronic condition, which means it requires long-term treatment. You may have to adapt other aspects of your lifestyle.
MAINTAINING A HEALTHY WEIGHT. Heart failure is often associated with rapid changes in weight. Losing a lot of
|
weight unintentionally over a short space of time can be serious. It could mean that you are not consuming enough calories or that your heart failure or inactivity are causing muscle loss. It could also indicate that your diuretic dose is too high.
SALT INTAKE. Reducing your salt intake can be important for people with heart failure. To reduce salt intake first remove the salt pot (shaker) from the table, than try to eat more fruit and vegetables, meat substitutes, unprocessed foods, low fat dairy products, polyunsaturated fats, cereals and fish.
FLUID INTAKE. For most patients with heart failure the amount of fluids that should be taken on a daily basis varies between 1.5 and 2 liters and it includes water, juice, ice cubes, coffee, milk, soup, tea or fizzy drtnks. To limit the amount you drtnk try using small cups instead of mugs, spread your daily allowance over the whole day and try drinking very cold or very hot or eat frozen fruits.
ALCOHOL INTAKE. Too much alcohol intake when you have an existing heart condition may raise your heart rate and blood pressure and long-term abuse may cause cardiomyopathy. In general it is recommended that you drink no more than 1 to 2 alcoholic beverages a day (a single drink is classed as one glass of beer or wine, or one mixed drink with only one measure of alcohol). If you have serious symptoms, you may be advised to avoid alcohol altogether.
 POTASSIUM INTAKE. If you are taking diuretics for your heart failure, your body may lose some of this potassium. Your doctor may prescribe you a type of diuretic or advise to supplement your diet with foods nch in potassium such as bananas, oranges, prunes, soybeans, cantaloupe melon, fish such as halibut or flounder and potatoes. POTASSIUM INTAKE. If you are taking diuretics for your heart failure, your body may lose some of this potassium. Your doctor may prescribe you a type of diuretic or advise to supplement your diet with foods nch in potassium such as bananas, oranges, prunes, soybeans, cantaloupe melon, fish such as halibut or flounder and potatoes.
FATS AND CHOLESTEROL. Your diet should include fruit and vegetables, fish, poultry, lean meat, meat- substitutes (e.g. soya), and unsaturated fats.
LIVING WITH HEART FAILURE
With the right care and support, heart failure should not keep you from doing most of the things you want to, as long as you are aware of your own limits.
ACTIVITY AND EXERCISE is beneficial for the majority of people with heart failure. Before starting an exercise program, or if you want to increase or change the type of exercise you do, talk to your doctor or nurse to make sure you are not putting too much strain on your heart too quickly. Always warm up and cool down with a few stretches before you begin exercising. If it is cold or windy outside, you should try and warm up before leaving the house. Walking is a good activity to start with. If you already walk, try cycling or swimming. Start slowly and gradually increases the distance or intensity of the activity as your strength/fitness improves. Stop exercising at once if you expenence shortness of breath, dizziness, chest pain, nausea or a cold sweat. Try not to exercise straight after a large meal, or when you haven't
|
eaten for a long time. Plan to exercise 1 -2 hours after a light meal. Activities that require holding your breath, beartng down or sudden bursts of energy are best avoided.
 SMOKING affects the oxygen carrying ability of your blood, contributes to the deposit of fats in your blood vessels, causing narrowing of vessels and increasing your blood pressure and causes the blood vessels to constrict (narrow). This will make the symptoms of your heart failure worse. It is never too late to stop smoking, and stopping will be beneficial for your heart. There are a number of different ways to stop smoking: 1. Use nicotine patches, gum and inhalers, 2. Give up gradually, reducing the number of cigarettes you have a day, 3. Brush your teeth after a meal instead of lighting a cigarette, 4. Avoid places where smoking is permitted, 5. Find something else to do with your hands or mouth, such as playing with a paperclip, or chewing gum, 6. Get more active, exercise boosts morale and helps you relax, 7. Don't empty your ashtray, this will show you how much you smoke and how horrid the smell of stale smoke is, 8. Involve your family, especially those who smoke - this can be key to success. SMOKING affects the oxygen carrying ability of your blood, contributes to the deposit of fats in your blood vessels, causing narrowing of vessels and increasing your blood pressure and causes the blood vessels to constrict (narrow). This will make the symptoms of your heart failure worse. It is never too late to stop smoking, and stopping will be beneficial for your heart. There are a number of different ways to stop smoking: 1. Use nicotine patches, gum and inhalers, 2. Give up gradually, reducing the number of cigarettes you have a day, 3. Brush your teeth after a meal instead of lighting a cigarette, 4. Avoid places where smoking is permitted, 5. Find something else to do with your hands or mouth, such as playing with a paperclip, or chewing gum, 6. Get more active, exercise boosts morale and helps you relax, 7. Don't empty your ashtray, this will show you how much you smoke and how horrid the smell of stale smoke is, 8. Involve your family, especially those who smoke - this can be key to success.
TRAVELING. If your heart failure is well-controlled and stable, you should have no difficulties with mild traveling. Sitting still for long periods in cramped positions in aircraft frequently leads to swollen ankles and sometimes muscle cramps. Regular stretching and mobility exercises can help, as well as walking around the cabin and while waiting in airports. In some cases, your doctor may recommend that you wear knee-high support stockings during the flight to prevent blood clots (DVT). It is very important that you remember to take all your medicines with you on holiday.
 DRIVING. Most people with heart failure can safely drive a car. However, people who have a history of loss of consciousness or fainting due to an abnormal heart rhythm (arrhythmia) in general should talk to their doctor about their ability to drive. People who drive for a living are likely to require regular review of their condition, and in some countries may be excluded from driving. Having a pacemaker will not prevent you from maintaining your driver's license. WORKING. In most cases, heart failure can be adequately treated and controlled, allowing you to continue to work full time for many years. Your particular situation will depend on the cause and severity of your heart failure, as well as the demands of your job. You may need to adjust your working hours or other strenuous activities. If you feel you are becoming less able to do your job, discuss this with your doctor in case a change of medication is needed, and/or with your employer to see if other work can be arranged. IMMUNIZATIONS. Respiratory infections like influenza (flu) or pneumonia, as respiratory problems can worsen heart failure. Safe vaccines that can provide immunity against flu and pneumonia are available. It n DRIVING. Most people with heart failure can safely drive a car. However, people who have a history of loss of consciousness or fainting due to an abnormal heart rhythm (arrhythmia) in general should talk to their doctor about their ability to drive. People who drive for a living are likely to require regular review of their condition, and in some countries may be excluded from driving. Having a pacemaker will not prevent you from maintaining your driver's license. WORKING. In most cases, heart failure can be adequately treated and controlled, allowing you to continue to work full time for many years. Your particular situation will depend on the cause and severity of your heart failure, as well as the demands of your job. You may need to adjust your working hours or other strenuous activities. If you feel you are becoming less able to do your job, discuss this with your doctor in case a change of medication is needed, and/or with your employer to see if other work can be arranged. IMMUNIZATIONS. Respiratory infections like influenza (flu) or pneumonia, as respiratory problems can worsen heart failure. Safe vaccines that can provide immunity against flu and pneumonia are available. It n |
RELATIONSHIPS. Effective management of heart failure is often a group effort. Your family members can play a key role in supporting you to live as actively as possible with your heart failure. Involve them in helping with aspects of your medical care issues, for ejxample helping with your medicine regime or measuring your heart rate and blood pressure. Consider ways in which you and your family can do activities together (for example, active family outings, preparing healthy meals together). Let it be known that you will accept help, but that you want to remain as independent as possible. SEX AND HEART FAILURE The most people with heart failure can continue to enjoy sexual relations once their symptoms are under control. You may feel more comfortable and confident when trying the following: 1. Choose a time for sex when you are rested, relaxed and not pressured, 2. Avoid having sex immediately after eating a heavy meal or drinking excessive amounts of alcohol, 3. Have sex in a comfortable, familiar room that is not too hot or too cold and where you will not be interrupted, 4. Use foreplay as a warm-up period to help your body get used to the increased activity level of intercourse, 5 .Have sex in less strenuous positions such as lying on the bottom or with you and your partner lying side by side. If at any time you start to feel uncomfortable, breathless or tired during intercourse, stop and rest for a short while. For problems such as erectile dysfunction (impotence) or problems with ejaculation there are very effective medical treatments available that most people with heart failure can use as required.
WARNING SIGNS It is important to monitor all your symptoms on a regular basis as heart failure can progress slowly. You should call for help immediately if you experience:
- Persistent chest pain that is not relieved by glyceryl trinitrate (GTN / nitroglycerin)
- Severe and persistent shortness of breath
- Fainting
You should inform your doctor as soon as possible if you experience: • Increasing shortness of breath
- Frequent awakenings due to shortness of breath
- Needing more pillows to sleep comfortably
- Rapid heart rate or worsening palpitations
And you should discuss any of the symptoms below with your doctor or nurse.
- Rapid weight gain
- Progressive swelling or pain in the abdomen
- Increased swelling of the legs or ankles
- Loss of appetite/nausea
- Increasing fatigue
- Worsening cough
You can find more about heart failure on
www.heartfailurematters.org
|